Management of diabetes and CKD should include nutritional intervention. Dietary modifications may reduce progression of CKD.
5.1 Target dietary protein intake for people with diabetes and CKD stages 1-4 should be the RDA of 0.8 g/kg body weight per day. (B)
Nutritional management for people with diabetes has traditionally focused on blood glucose control. However, dietary protein intake at all stages of CKD appears to have an important impact in this population. If dietary protein is limited, adequate caloric intake must be maintained by increasing calories from carbohydrates and/or fats. Competing needs for nutritional management of hyperglycemia, hypertension, and dyslipidemia can make determination of appropriate protein intake challenging. Furthermore, the diet for diabetes and CKD should consider the qualitative, as well as the quantitative, aspects of proteins, carbohydrates, and fats. To address dietary recommendations for people with diabetes and CKD stages 1 to 4, studies evaluating interventions that reduced or altered sources of dietary protein and other nutrients were reviewed (Table 37 to Table 41). Dietary recommendations for CKD stage 5 are provided in the KDOQI™ CPGs for Nutrition in Chronic Renal Failure.9
A dietary protein intake of 0.8 g/kg body weight per day, the RDA for this macronutrient, is a level that has been achieved in studies of diabetes and CKD. Reduction in albuminuria and stabilization of kidney function have been reported with dietary protein intake at the RDA level. Nutrition surveys indicate that most people eat in excess of the RDA for dietary protein. (Moderate)
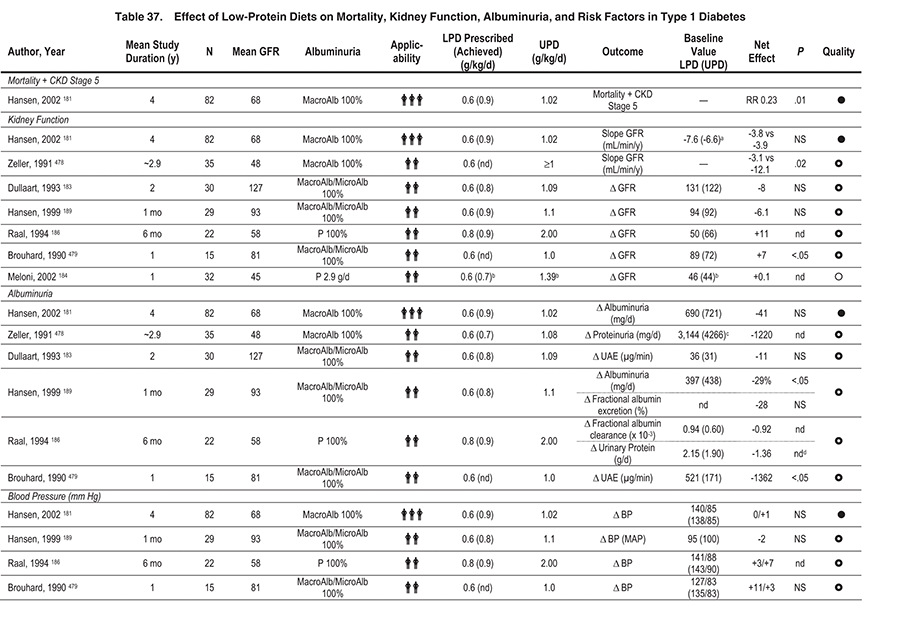
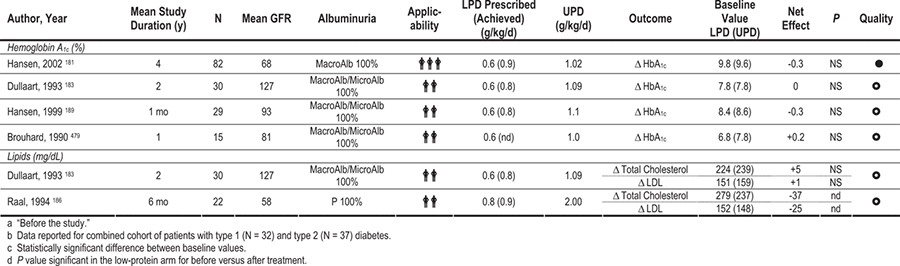
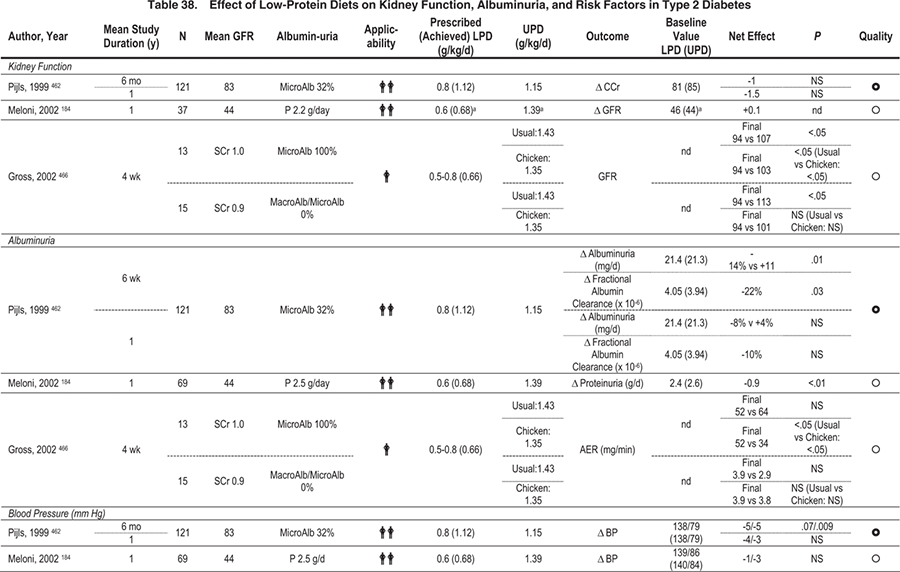
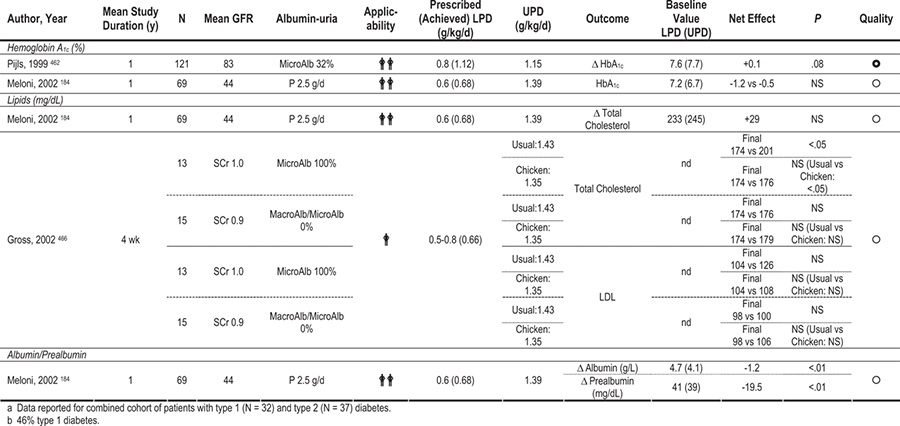
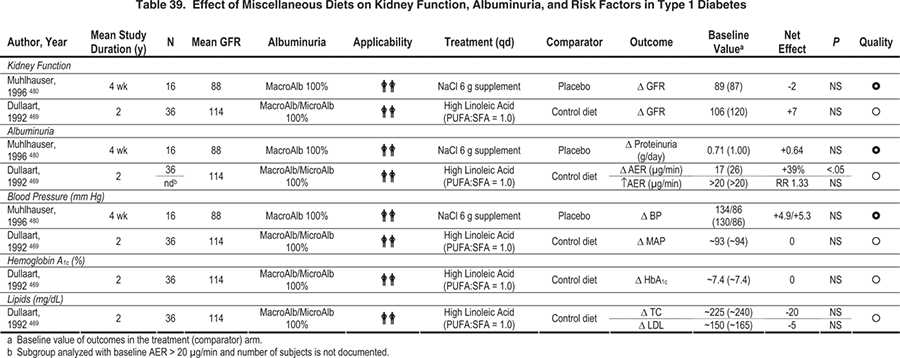
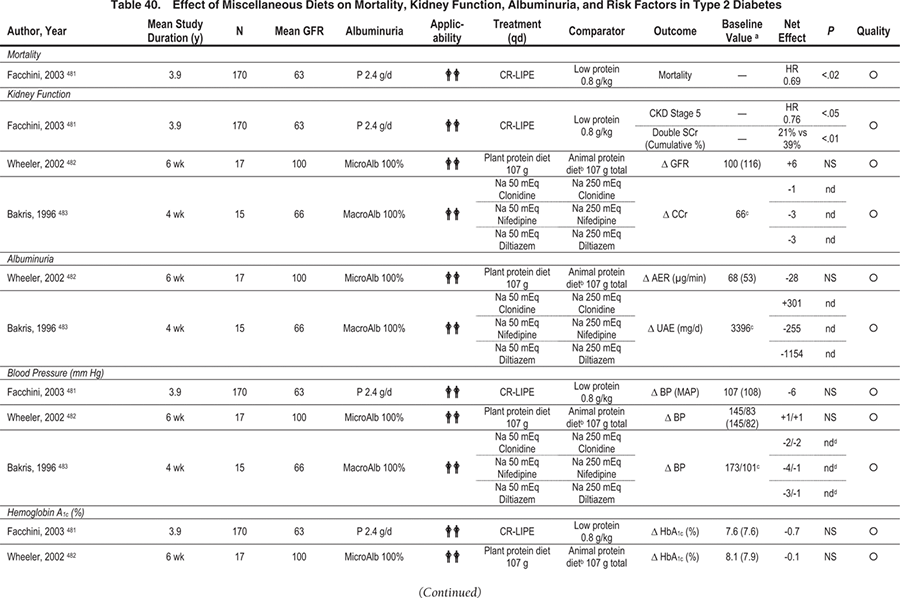
Key studies that evaluated reduction or alteration of dietary protein are summarized in Table 42. Based on 2 meta-analyses, low-protein diets reduced risks of loss of kidney function (GFR or creatinine-based measurements) and/or increased albuminuria (measured as urinary excretion of either albumin or total protein), with more pronounced benefits in DKD than in non-DKD (Fig 21). 179,180 More recently, even a modest limitation of dietary protein (0.89 versus 1.02 g/kg body weight per day) substantially reduced the risk of CKD stage 5 or death (RR, 0.23; 95% CI, 0.07 to 0.72; P = 0.04) in people with type 1 diabetes and CKD stage 2 (inferred based on levels of albuminuria and GFR; Fig 22). These patients (85% to 89% during the course of the study) also received ACE inhibitors and had similar control of blood pressure and other risk factors irrespective of diet group assignment, indicating that reducing dietary protein provided benefits beyond established medical therapies.181 Benefits of limiting dietary protein intake are more evident in type 1 than type 2 diabetes, but fewer studies have been done in the latter population. Based on the available evidence (Table 37 and Table 38), the Work Group concluded that limiting dietary protein will slow the decrease in kidney function and progression of albuminuria, and it may prevent CKD stage 5.
At the other end of the spectrum, high-protein diets are a particular concern in patients with diabetes because they increase albuminuria and may accelerate loss of kidney function. Glomerular hyperfiltration and increased intraglomerular pressure are well-recognized mechanisms of kidney damage induced by excess dietary protein. Based on both human studies and experimental models, higher protein intake appears to have more pronounced effects on kidney hemodynamics and kidney damage in diabetes.187-196,463 Emerging epidemiological evidence indicates that higher protein intake (≥20% versus 10% of total daily calories) is associated with loss of kidney function in women with mild kidney insufficiency (defined as estimated GFR < 80 and > 55 mL/min/1.73 m2) and development of microalbuminuria in people with diabetes and hypertension.197,198 Therefore, in the opinion of the Work Group, people with diabetes and CKD should avoid high-protein diets (≥20% of total daily calories). Some common fad diets that recommend high protein are Atkins®, Protein Power, the Zone, South Beach®, and Sugar Busters®.


Diets for people with diabetes have traditionally been 15% to 20% protein.464 The NHANES 1999 to 2000 indicated that the majority of Americans consume 15% of total daily calories or approximately 1.04 g/kg body weight per day as protein, substantially more than the 0.8 g/kg body weight per day RDA.178 In the DASH and DASH-Sodium diets, a higher protein intake (1.4 g/kg body weight per day) is recommended.199 However, sources of protein in the DASH diets emphasize vegetables, low-fat or nonfat dairy products, whole grains, nuts, legumes, fish, and poultry. Red meat is eaten in only small amounts. In recent studies of people with prehypertension or untreated stage 1 hypertension, higher protein intake from either soy or predominantly vegetable sources reduced blood pressure in short-term (6 to 12 weeks) feeding studies.200, 201 Along with the DASH trials, these data suggest that predominantly nonmeat protein may have a beneficial effect on blood pressure. However, whether the blood pressure effect is due to the protein content or other dietary components, such aspotassium or isoflavones, is unknown.465 Several small studies indicate that vegetable or soy protein sources also may be kidney sparing compared with red-meat sources in diabetes and CKD, and in the Nurses Health Study, the risk of losing kidney function in women with mild kidney insufficiency was related primarily to animal meat intake.182, 185, 197, 202, 466 Higher dairy or vegetable protein intake did not increase this risk. Therefore, a DASH-type diet that emphasizes sources of protein other than red meat may be a reasonable alternative to a lower total protein intake in people with hypertension, diabetes, and CKD stages 1 to 2. Nevertheless, people who achieve the RDA for protein, 0.8 g/kg body weight per day, and maintain an adequate caloric intake remain well nourished. Regardless of the level of protein intake, 50% to 75% of the protein should be of high biological value, derived predominantly from lean poultry, fish, and soy- and vegetable-based proteins.
If dietary protein intake is limited, an increase in carbohydrates and/or fats is required for adequate caloric intake. Increasing intake of omega-3 and monounsaturated fats may confer benefits on CKD. (Weak/Opinion)
Evidence of biological activity of dietary fats and carbohydrates indicates that an exclusive focus on protein is too limiting with regard to broad effects on health in people with diabetes and CKD. When protein intake is limited, caloric distribution of the other macronutrients must be addressed. According to the National Academy of Sciences, Institute of Medicine, nonprotein calories (90% of total) should be distributed as 30% or less from dietary fats and up to 60% obtained from complex carbohydrates.467 The ADA recommends that carbohydrates be derived primarily from whole grains, fruits and vegetables, and nonfat or low-fat dairy products.174 Although glycemic effects are determined strongly by total amount of carbohydrate, low-glycemic index foods (a measure of type of carbohydrate) may decrease postprandial hyperglycemia and improve overall blood glucose control.174 Dietary fiber is encouraged and may produce metabolic benefits on glycemia and lipids.174
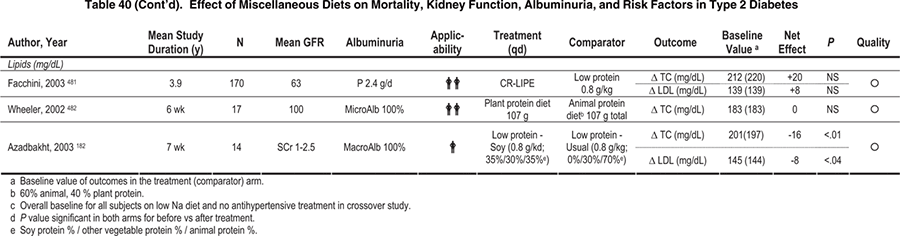
The optimal distribution of calories between fatty acid classes remains to be determined. Recommendations for fatty acids usually combine polyunsaturated fatty acids together without differentiating between categories. Few studies have examined the effects of fatty acid intake or supplements on markers of kidney disease and risk factors in patients with diabetes (Table 41).468-472 Moreover, these studies were short term and performed in small numbers of people, precluding firm conclusions. Nevertheless, the available evidence suggests that increased intake of omega-3 and monounsaturated fatty acids may be considered because of potentially favorable effects on progression of CKD (Table 41). Fatty acid intake can be modified easily by substituting canola oil, a blend that includes both omega-3 and monounsaturated fats, for vegetable oils. Several brands of salad dressings and butter replacement products made from canola oil are available in most grocery stores. To reduce intake of saturated fat, consumption of red meats should be reduced, and low-fat or nonfat dairy products should be used.
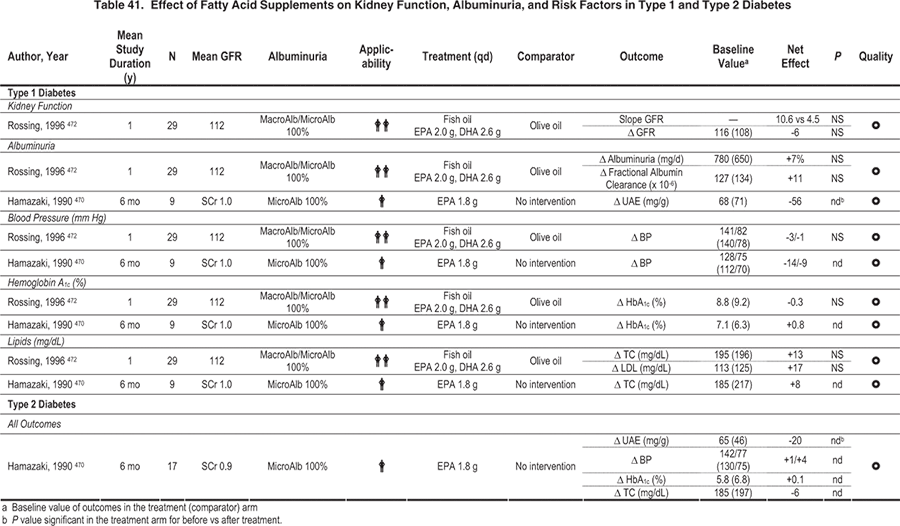
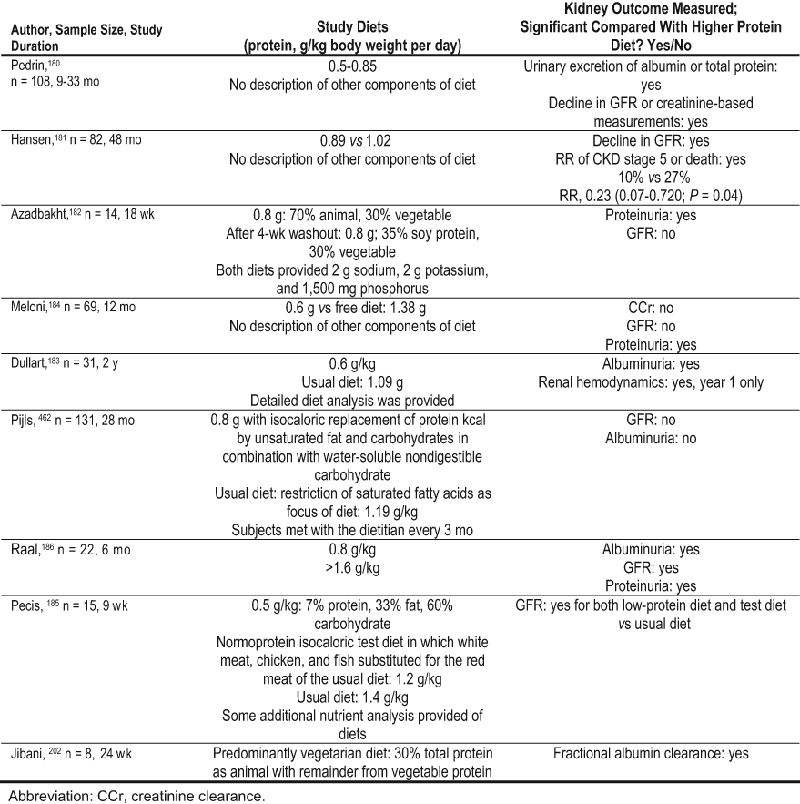
Table 42. Key Studies Evaluating Effects of Dietary Protein Restriction or Other Alterations on Kidney Outcomes in Patients With Diabetes and CKD
People with diabetes and CKD should receive intervention from a specialty-trained registered dietitian that includes individualized management of multiple nutritional aspects. (Moderate)
The diet for diabetes and CKD is more complicated than that for either condition alone. The management of diabetes and CKD involves multiple nutrients (macronutrients and micronutrients), including protein, carbohydrate, fat, sodium, potassium, and phosphate, among many others. Nutritional intervention should be individualized and completed in an interactive manner. Patients should identify achievable goals and lifestyle behaviors they want to modify. Several studies have documented that frequent patient contact with a registered dietitian accomplishes dietary goals and/or improves clinical outcomes.45, 473-475 This finding includes studies of patients with microalbuminuria and diabetes,45 dialysis patients who have diabetes,474 and patients with decreased GFR.475 Because this observation applies across a wide spectrum of patients, those with diabetes and CKD at all stages are likely to benefit from interaction with a registered dietitian.
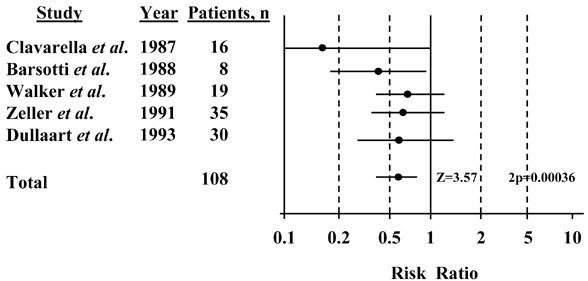
Figure 21. Meta-Analysis Demonstrating Reduced Risk of Progression of DKD (Loss of Kidney Function or Increased Albuminuria) by Treatment with Low-Protein Diets. Reprinted with permission.180
The NKF-KDOQI™ Guidelines on Hypertension and Antihypertensive Agents in CKD recommended a version of the DASH diet with modifications for CKD stages 3 to 4.5,199 These modifications decreased dietary protein from 1.4 g/kg body weight per day to 0.6 to 0.8 g/kg body weight per day, as well as restricted phosphorus (0.8 to 1.0 g/d) and potassium (2 to 4 g/d).5 Based on concerns about potential detrimental effects of high-protein diets on the kidney and evidence for kidney and survival benefits at approximately the RDA level in diabetes and CKD stages 1 to 2, the Work Group concluded that a protein intake that meets, but does not exceed, the RDA would be prudent at earlier stages of CKD (Table 43). The ADA endorses a dietary protein intake of 0.8 g/kg body weight per day for people with DKD.34 An additional restriction to 0.6 g/kg body weight per day is suggested should glomerular filtration rate begin to decrease. The dietary protein recommendation should be based on idealized body weight because obesity, which is highly prevalent in the diabetes and CKD population, otherwise would lead to overestimating the dietary protein recommendation.
Dietary sodium reduction to 2.3 g/d (100 mmol/d) is recommended based on the DASH and DASH-Sodium diets.199 Because most people with diabetes and CKD have hypertension characterized by enhanced sodium retention, this limitation should apply. Recommendations for phosphorus and potassium are the same for CKD with and without diabetes. Phosphorus binders may be needed in patients with advanced CKD because of the emphasis on whole grains and dairy products.
The Institute of Medicine established guidelines for intake of omega-3 fatty acids, which recognize significant variances in physiologicalpotency between different omega-3 fatty acids. Adequate intake of alpha-linolenic acid was established as 1.6 g/d for men and 1.1 g/d for women, with substitution of up to 10% of these amounts by the more physiologically potent eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA).467 The AHA and the KDOQI™ CPGs for CVD in Dialysis Patients recommend including 1 serving of cold-water fish in the diet 3 times per week.10, 476 It is possible that 3 servings of cold-water fish, such as salmon, mackerel, herring, and albacore tuna, would provide EPA and DHA in excess of the 10% of adequate intake amounts for men and women. The Work Group is not aware of studies indicating disadvantages from this amount of EPA or DHA. However, some concerns exist related to the potential for unacceptable levels of mercury or other contaminants. Nevertheless, in the opinion of the Work Group, these recommendations may be considered for the diabetes and CKD population.
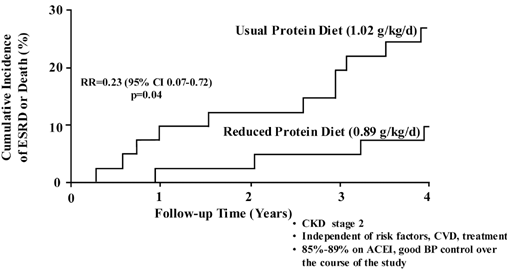
Figure 22. Effect of Reduced Dietary Protein Intake on CKD Stage 5 and Death in Type 1 Diabetes and CKD Stage 2 (inferred) at baseline.
Reprinted with permission.181
Table 43. A Balanced Approach to Nutrition in CKD With or Without Diabetes: Macronutrient Composition and Mineral Content

Studies of dietary protein interventions in diabetes and CKD are relatively few, short term, completed in small numbers of participants, and have limited documentation of DKD. In addition, both the qualitative (eg, beef, chicken, or soy sources) and quantitative definition of a low-protein diet differ tremendously among studies. Substantial differences in amounts and types of fat and carbohydrate also have not been acknowledged adequately. This type of variability is a potential explanation for the inconsistent results observed between studies evaluating the effect of protein intake on kidney outcomes.
As detailed in CPR 4, adherence to nutritional regimens is particularly challenging. Therefore, methods to improve adherence are crucial to achieve nutritional goals. In addition, diets recommended by health care professionals often are viewed as unpalatable and unattractive. Culinary approaches to enhance appeal of nutrient-appropriate foods should be encouraged, along with methods to make food preparation easy and inexpensive. An example of a meal plan that meets the nutritional goals of this guideline is provided in Appendix 1. A professional chef designed the menu and accompanying recipes in collaboration with registered dietitians experienced with diabetes and CKD. In the view of the Work Group, these types of creative approaches facilitate interest and feasibility for lifestyle modification in diabetes and CKD.
Schedule for Nutritional Assessment and Intervention
The Renal Dietitians Dietetic Practice Group of the American Dietetic Association recommends nutritional assessment and intervention at the diagnosis of CKD and quarterly thereafter.477Considering that diabetes further complicates CKD care, frequency of assessment may be adjusted based on the needs of individual patients. A registered dietitian who is knowledgeable of both conditions should perform nutritional assessments and interventions. Obtaining accurate dietary histories often is challenging because of the subjective nature of reporting and difficulty with recall. For some key nutrients in the regimen recommended for diabetes and CKD, such as sodium and protein (estimated by urinary urea nitrogen excretion), 24-hour urine studies are useful to assess intake and guide counseling. Close monitoring of patients who follow a dietary protein restriction is important to ensure adequate, but not excessive, protein intake.